
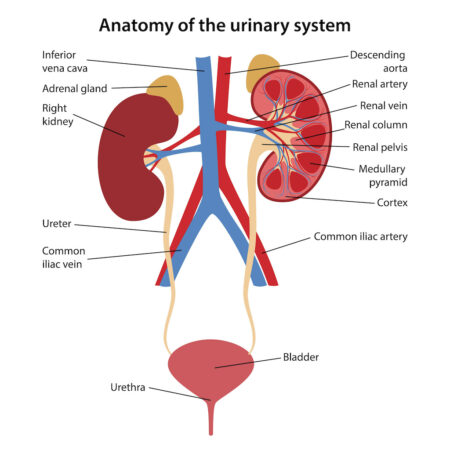
 The kidneys are remarkable and complex organs that serves many essential functions.
The kidneys are remarkable and complex organs that serves many essential functions.
Essential kidney functions:
- Remove protein wastes and toxins from the body.
- Balance the body’s fluids.
- Keep electrolytes at optimal levels.
- Control pH levels of the blood
- Release hormones that regulate blood pressure.
- Maintain the production of red blood cells.
Kidney disease occurs when one or more of these essential functions are compromised or reduced. When kidney function is impaired, body systems become imbalanced. When function is significantly impaired, waste levels can become toxic. Kidney disease can progress to kidney failure.
Causes of Kidney Disease
Infections – Bacterial infections that can cause kidney failure in dogs include Leptospirosis and Lyme disease. Leptospirosis is contacted through urine contaminated drinking water. Lyme disease is acquired through the bite of a deer tick. Both cats in dogs can also acquire ascending infections from the lower urinary system. Untreated bladder infections can cause kidney infections.
Toxicity – The kidney is susceptible to adverse toxicity reactions due to its role in filtering the blood. Common toxins that can cause acute kidney failure include grapes/raisins (dogs), antifreeze, rodenticides, Ibuprofen, and lilies (cats).
Cancers – Renal carcinoma is the most common primary renal tumor in dogs and cats. These tumors have aggressive malignancies with the potential for widespread metastasis. Cancers, including lymphoma, can also originate in other parts of the body and metastasize to the kidneys.
Congenital – Inherited malformation of the kidneys can present in pets under a year of age. The most common condition is polycystic kidney disease in Persian and domestic long-haired cats. The condition causes multiple fluid filled cysts to form within the functional part of the kidney.
Immune Mediated – Glomerulonephritis occurs when a mixture of antibodies and pathogens are filtered out of the bloodstream. When these compounds are trapped, the body responds by activating its immune defenses, resulting in damage to the kidney tissue.
Urinary Obstruction – Stones may form in the kidneys or bladder. If the stones move from the kidneys into the ureters or from the blader into the urethra, an obstruction that impedes the flow of urine may result. Restricted urine flow can cause a secondary kidney failure.
Chronic Disease – Many senior pets experience a gradual loss of kidney function over time. For older animal populations kidney disease affects up to 10% of dogs and 35% of cats. The exact inciting incident or cause is often not identified in these patients.
 Clinical Signs
Clinical Signs
Kidney disease may be detected on routine screening of blood and urine prior to the onset of clinical signs.
A few signs to watch for include:
- Drinking more water
- Increase in urine frequency or volume
- Loss of interest in playing
- Decrease in appetite
- Vomiting
- Weight & muscle loss
- Poor haircoat
- Bad breath
Unfortunately, kidney disease typically goes undetected and clinical signs do not appear until the kidneys are functioning at 33% or less of original capacity.
Diagnostic Tests
Diagnosis of kidney disease may require a variety of tests including blood work, urine tests, imaging, and blood pressure.
Blood Tests
Biochemistry Panel – BUN, CREA, and SDMA are measured by a blood chemistry test. Elevations (azotemia) can indicate the kidneys’ declining ability to filter the blood.
Electrolytes & Minerals – Levels of blood electrolytes including potassium, sodium, and chloride may be abnormal. Minerals such as calcium and phosphorous may also be elevated.
CBC – Evaluates levels of red blood cells to look for anemia and white blood cells to identify infection.
Titers – Blood tests for infection including Lyme Disease and Leptospirosis in dogs.
 Urine Tests
Urine Tests
Urinalysis – Analysis of urine by physical, chemical, and microscopic means to test for the presence of disease.
Urine Culture & Susceptibility – The best test to diagnose a urinary tract infection is a culture to grow and identify bacteria present in the urinary tract. The bacteria are then further tested to determine the best antibiotic to use in treatment of the infection.
Urine Protein/Creatinine Ratio – A simple test that measures how much protein is being lost through the kidneys.
Imaging
X-Rays – Radiographs help to assess the size and shape of the kidneys. Kidney enlargement, atrophy or shrinkage, and abnormal shapes or asymmetry may indicate disease. The presence of masses or tumors that change the shape of the kidney can sometimes be visualized using radiographs. Kidney and bladder stones may also be identified on x-rays.
Ultrasound – Ultrasonography is the best diagnostic imaging modality to evaluate the internal structure of the kidneys. Ultrasound reveals any changes in the internal anatomy of the kidney, including abnormal growths, stones, or blood flow.
Blood Pressure – Monitoring blood pressure in kidney patients is important. High blood pressure (hypertension) is a very common symptom associated with chronic kidney disease. Hypertension causes further deterioration of kidney function.
Classifications and staging
Kidney disease in pets can be classified as acute or chronic. Acute kidney failure happens quickly over several days, and is often a result of sudden kidney injury caused by a specific event such as toxin, obstruction, or infection. Chronic kidney failure happens slowly over months to years. Chronic kidney disease is more prevalent in senior pets and progresses with age.
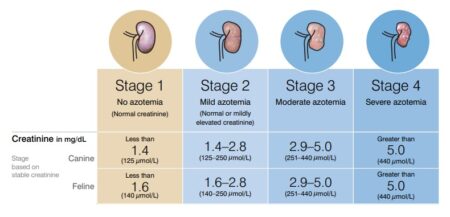
Kidney disease is staged based upon results of diagnostic tests including the level of nitrogen waste build up (azotemia), amount of protein in the urine, and blood pressure. The stage of disease helps to guide therapy and to determine prognosis.
Treatment Options
Although there is no definitive cure for kidney disease, treatment can often improve and prolong the lives of pets with this disease. Therapy is geared toward minimizing the buildup of toxic waste, maintaining hydration, addressing disturbances in electrolytes, supporting appropriate nutrition, controlling blood pressure, and slowing the progression of kidney disease.
 Nutritional Therapy – Prescription therapeutic foods, such as Science Diet KD or Purina NF, are formulated with low levels of phosphorous and moderate amounts of high quality protein. These diets are highly palatable and calorie dense to support debilitated animals. Prescription renal diets have domonstrated in studies to prolong survival time, slow disease progression, and improved quality of life.
Nutritional Therapy – Prescription therapeutic foods, such as Science Diet KD or Purina NF, are formulated with low levels of phosphorous and moderate amounts of high quality protein. These diets are highly palatable and calorie dense to support debilitated animals. Prescription renal diets have domonstrated in studies to prolong survival time, slow disease progression, and improved quality of life.
Hydration – Kidney disease patients are prone to dehydration due to body’s inability to conserve water. Patients must always have free access to water. Severely dehydrated patients may need to be hospitalized for IV fluids. Moderate chronic dehydration may be treated with subcutaneous fluids, which are fluid injections under the skin. Feeding of canned food can naturally increase daily water intake for pets experiencing mild dehydration.
Supplements – Additional potassium supplementation may be needed in some cats with chronic kidney disease. Control of blood phosphorus levels is also necessary. If dietary changes alone do not accomplish this, drugs to bind the phosphorus in the food can be given with each meal.
Detox – With acute toxin exposures, a veterinarian can take steps to minimize absorption of toxins. Depending on the situation, the veterinarian may induce vomiting or pump a pet’s stomach, administer activated charcoal, and administer an appropriate antitoxin.
Medications – Patients with acute infectious causes of kidney disease should be treated with broad-spectrum antibiotics. Ideally, the antibiotic choice should be based on test results including titer and bacterial culture. Pets that have poor appetites or nausea may benefit from antacid and anti-nausea medications, such as famotidine and Cerenia. If hypertension and proteinuria is present, a variety of drugs, such as Ace inhibitors, can be used to control the high blood pressure.
Prognosis
The prognosis for pets with kidney disease varies depending on the inciting cause, timeliness of diagnosis, and therapy provided.
Early diagnosis and intervention are important for successful treatment of dogs and cats with kidney disease. Pets that have a delayed diagnosis will have a poorer prognosis and may only live weeks to months. Patients that are diagnosed in the early stages of disease can live several years with conscientious management of their disease by the veterinarian and pet owner. On average cats tend to live longer than dogs with kidney disease.
In most cases, kidney disease is a progressive disease that worsens over time, but the rate of progression is highly variable. Regular follow up exams and lab tests help the veterinarian determine the progression of an individual animal’s kidney disease and make tailored changes in medical management.
Successful treatment of kidney disease delays progression, provides greater survival times, and increases patient quality of life.








 What causes IVDD
What causes IVDD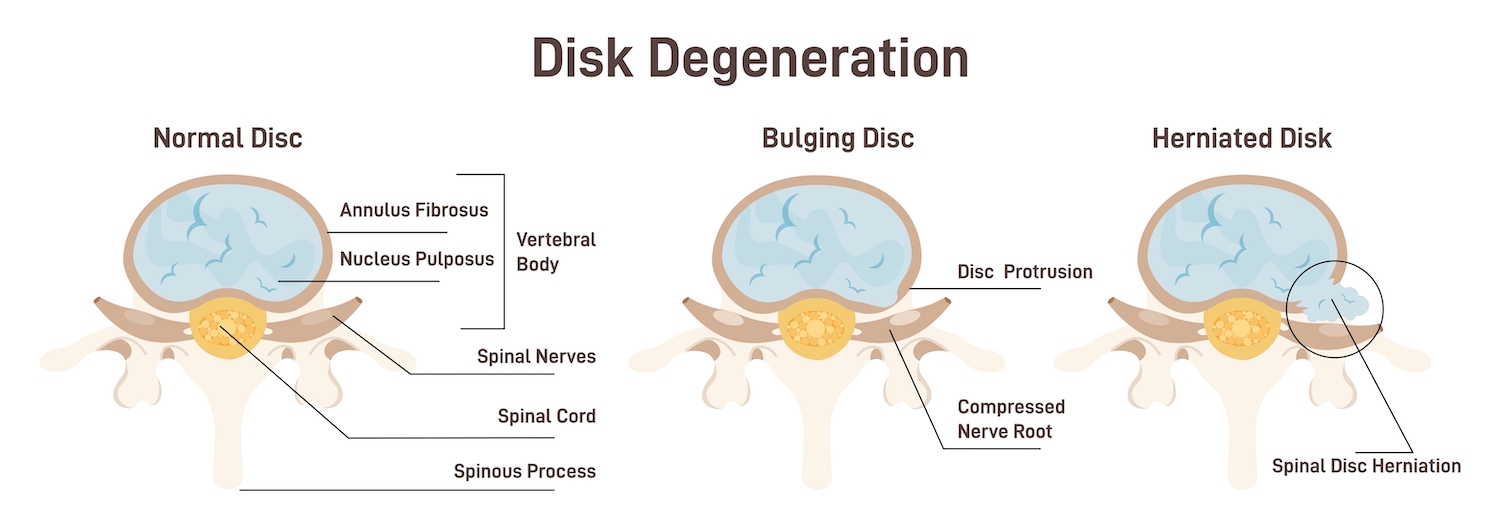
 Diagnosis of IVDD
Diagnosis of IVDD Prognosis of IVDD
Prognosis of IVDD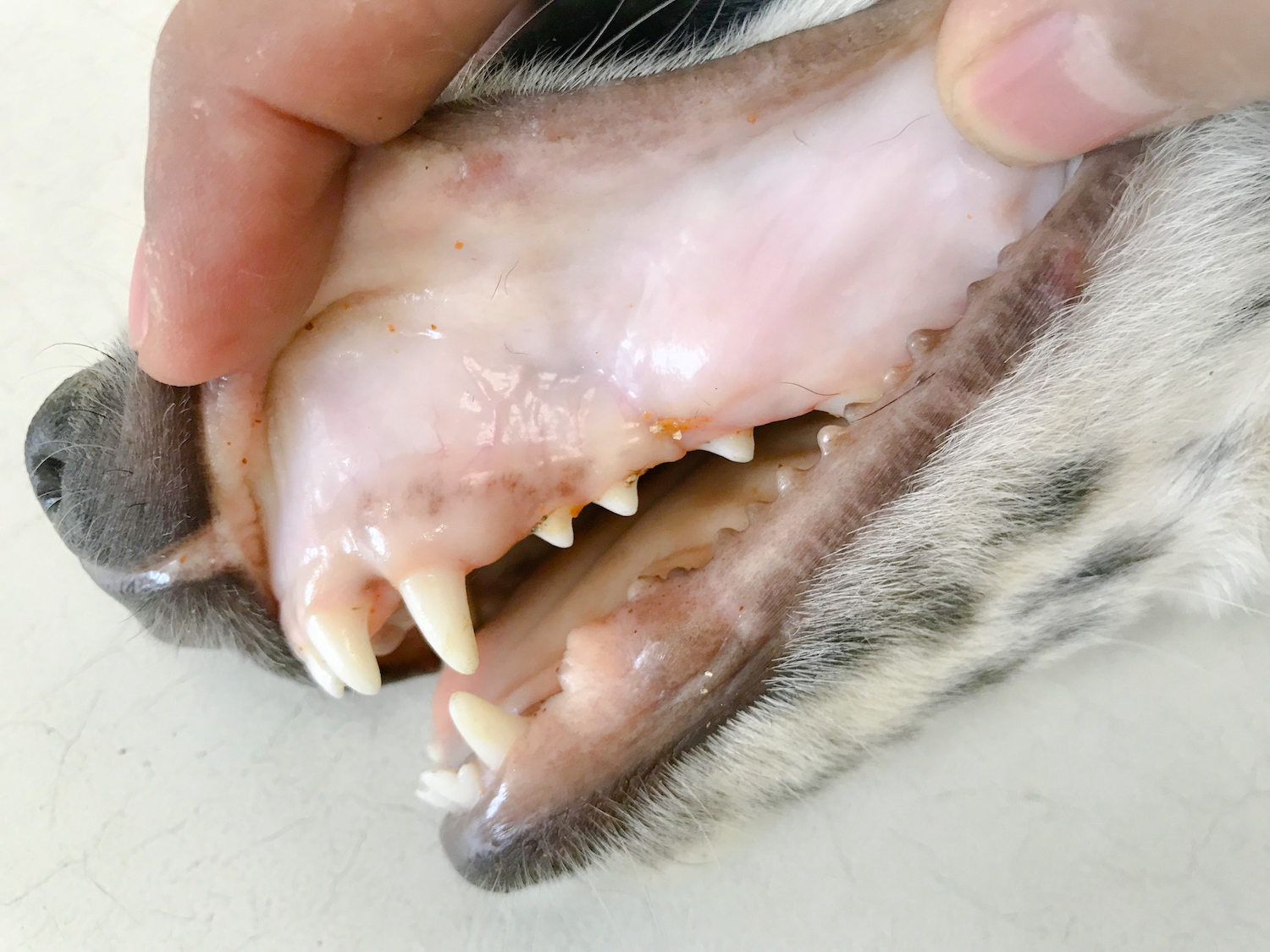
 Causes and Toxicity
Causes and Toxicity Clinical Signs
Clinical Signs Treatment
Treatment Prevention
Prevention
 Fleas are insects that consume blood from mammal hosts. Adult fleas are tiny, measuring only 2.5 mm long. Their bodies are shiny and reddish brown in color. Fleas do not have wings, but they can jump long distances. Several species of fleas can infest pets, but the most common one found on cats & dogs is the cat flea or Ctenocephalides felis. Fleas are a public health concern because they can
Fleas are insects that consume blood from mammal hosts. Adult fleas are tiny, measuring only 2.5 mm long. Their bodies are shiny and reddish brown in color. Fleas do not have wings, but they can jump long distances. Several species of fleas can infest pets, but the most common one found on cats & dogs is the cat flea or Ctenocephalides felis. Fleas are a public health concern because they can 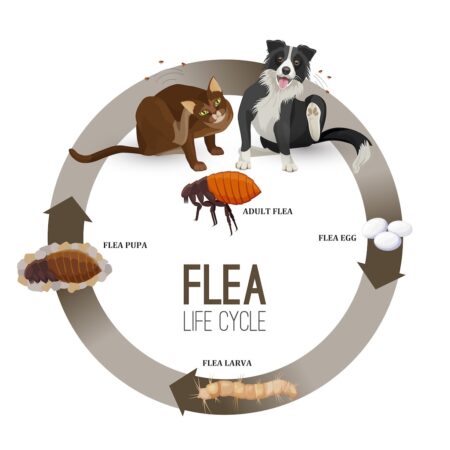 Flea Life Cycle
Flea Life Cycle Symptoms & Diagnosis
Symptoms & Diagnosis Prevention
Prevention 
 Symptoms of Feline Urinary Disease
Symptoms of Feline Urinary Disease Treatment of FLUTD
Treatment of FLUTD Improve Liter Box Accommodations
Improve Liter Box Accommodations Increase Water Intake
Increase Water Intake
 Causes
Causes Diagnosis
Diagnosis Follow-up
Follow-up
 The kidneys are remarkable and complex organs that serves many essential functions.
The kidneys are remarkable and complex organs that serves many essential functions. Clinical Signs
Clinical Signs Urine Tests
Urine Tests
 Nutritional Therapy – Prescription therapeutic foods, such as Science Diet KD or Purina NF, are formulated with low levels of phosphorous and moderate amounts of high quality protein. These diets are highly palatable and calorie dense to support debilitated animals. Prescription renal diets have domonstrated in studies to prolong survival time, slow disease progression, and improved quality of life.
Nutritional Therapy – Prescription therapeutic foods, such as Science Diet KD or Purina NF, are formulated with low levels of phosphorous and moderate amounts of high quality protein. These diets are highly palatable and calorie dense to support debilitated animals. Prescription renal diets have domonstrated in studies to prolong survival time, slow disease progression, and improved quality of life. 
 No amount of chocolate is safe for an animal to ingest. The effects of chocolate consumption in pets depends on type of chocolate, quantity consumed, and the size (body weight) of the pet. Some types of chocolate contain higher amounts of caffeine and theobromine.
No amount of chocolate is safe for an animal to ingest. The effects of chocolate consumption in pets depends on type of chocolate, quantity consumed, and the size (body weight) of the pet. Some types of chocolate contain higher amounts of caffeine and theobromine. Treatment of Chocolate Toxicity
Treatment of Chocolate Toxicity
 Diagnostic Tests
Diagnostic Tests Treatment Options
Treatment Options Follow-up Care
Follow-up Care
Recent Comments